Quick Tips: Getting Active as a Family
When the whole family is involved in physical activities together, children learn that being active is fun and makes you feel good. And busy parents can combine family time with exercise time.
Try these tips for getting everyone in the family up and moving together:
Getting started
- As a family, make a list of activities you’d like to do together.
- Make sure the activities are things everyone can do and enjoy.
- Keep a family physical activity log, or hang a calendar on the wall.
- Try to plan one or two family activities a week. For ideas, see the suggestions below.
- Once a month, plan something special that involves being active, like a trip to the zoo, a day hike, or camping.
- Use a safe backpack, stroller, or bike trailer so that smaller children can be included in family activities.
Walking
When family schedules get really busy, going for a walk may be the easiest thing you can do together.
- Start with short walks that everyone in the family can do. Add more distance gradually. Younger children can ride a bike or a tricycle. You can pull a wagon in case little ones get tired.
- Scavenger hunts can keep children from being bored on a walk. Keep in mind a list of “treasures” they can find, such as a red leaf, a blue house, a black dog, or an out-of-state license plate.
- Use a phone app or get pedometers, and work on increasing the number of steps you take on your family walks. Start with a goal of 10,000 steps a day.
- Register the whole family in a family fun run/walk in your community. If the event is for charity, have your family walk through your neighborhood to collect pledges.
Outdoor activities
- Go for a bike ride.
- Join your children in old-fashioned games like hopscotch, tag, jump rope, and hide-and-seek.
- Get involved in family-friendly sports like skiing, skating, swimming, and tennis.
- Play a daily family basketball game in the driveway or at a playground.
- Take up miniature golf or flying-disc golf.
- Fly a kite.
- Pick up trash at a local park.
Indoor and rainy-day activities
- Have a family dance night. Share dances from each generation, and teach each other to do them. Or learn folk dances.
- Create a new dance or exercise routine to a favorite song. Have a different child choose the song each week.
- Go to the mall, and count how many laps you can walk as a family.
- Have a hula hoop contest.
- Set up a fun obstacle course in the basement, garage, or spare room.
General rules
- Limit TV, video games, and computer time.
- Don’t use food as a reward for meeting activity goals.
- Make physical activity a priority. Don’t let things get in the way of family activity time.
To view this article on Healthwise, click here
©1997–2019, Healthwise, Incorporated
 There’s nothing quite like a good comeback. It’s a testament to the determination of the human spirit, and a reminder of why second chances can be a great thing. The beauty of a comeback is that it happens in many forms. It could be an athlete getting back on the field after a major injury, or a determined older student going back to school to finally earn their degree. For Adam McCullough, it’s finding his way back into the driver’s seat.
There’s nothing quite like a good comeback. It’s a testament to the determination of the human spirit, and a reminder of why second chances can be a great thing. The beauty of a comeback is that it happens in many forms. It could be an athlete getting back on the field after a major injury, or a determined older student going back to school to finally earn their degree. For Adam McCullough, it’s finding his way back into the driver’s seat.
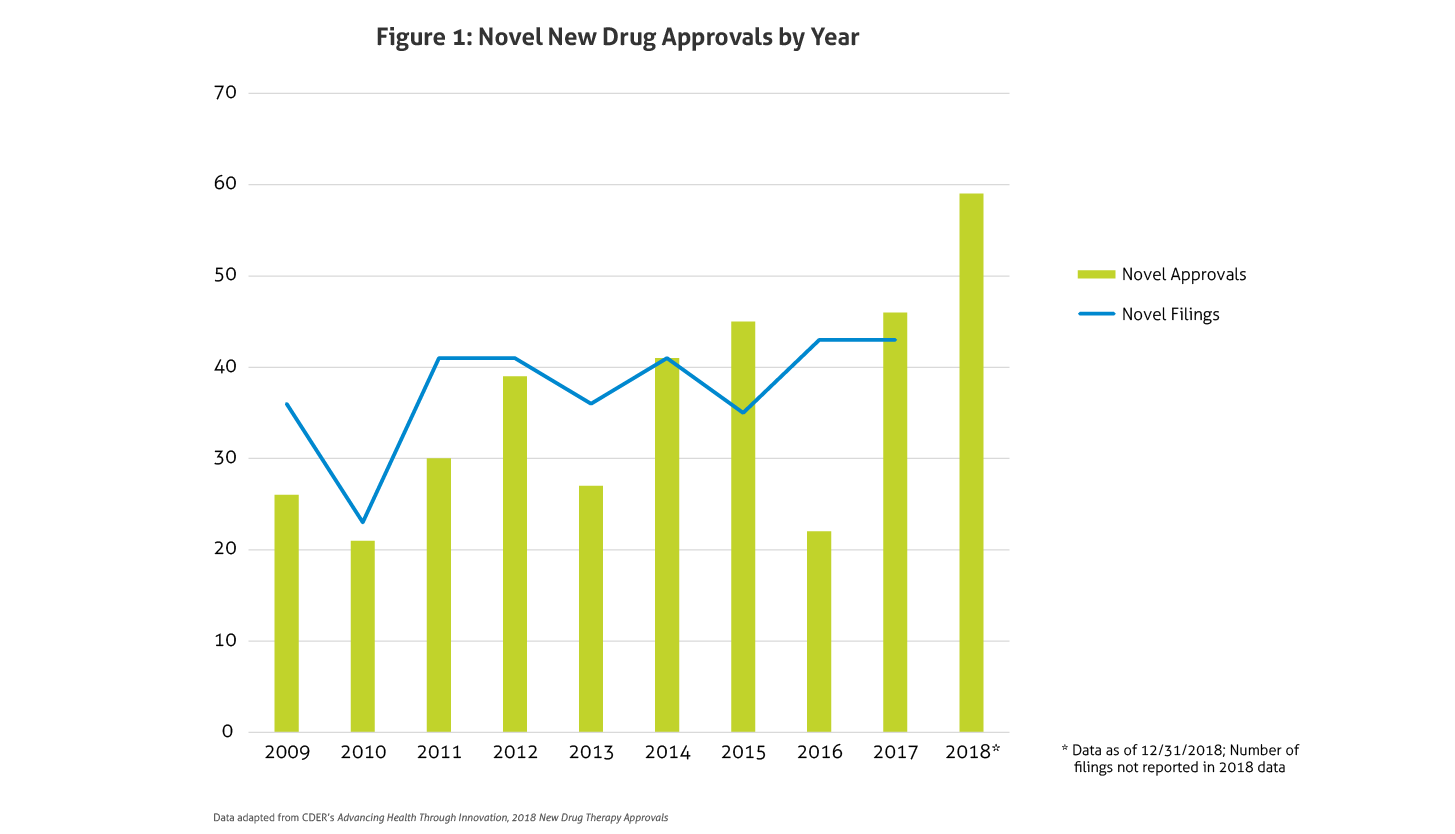
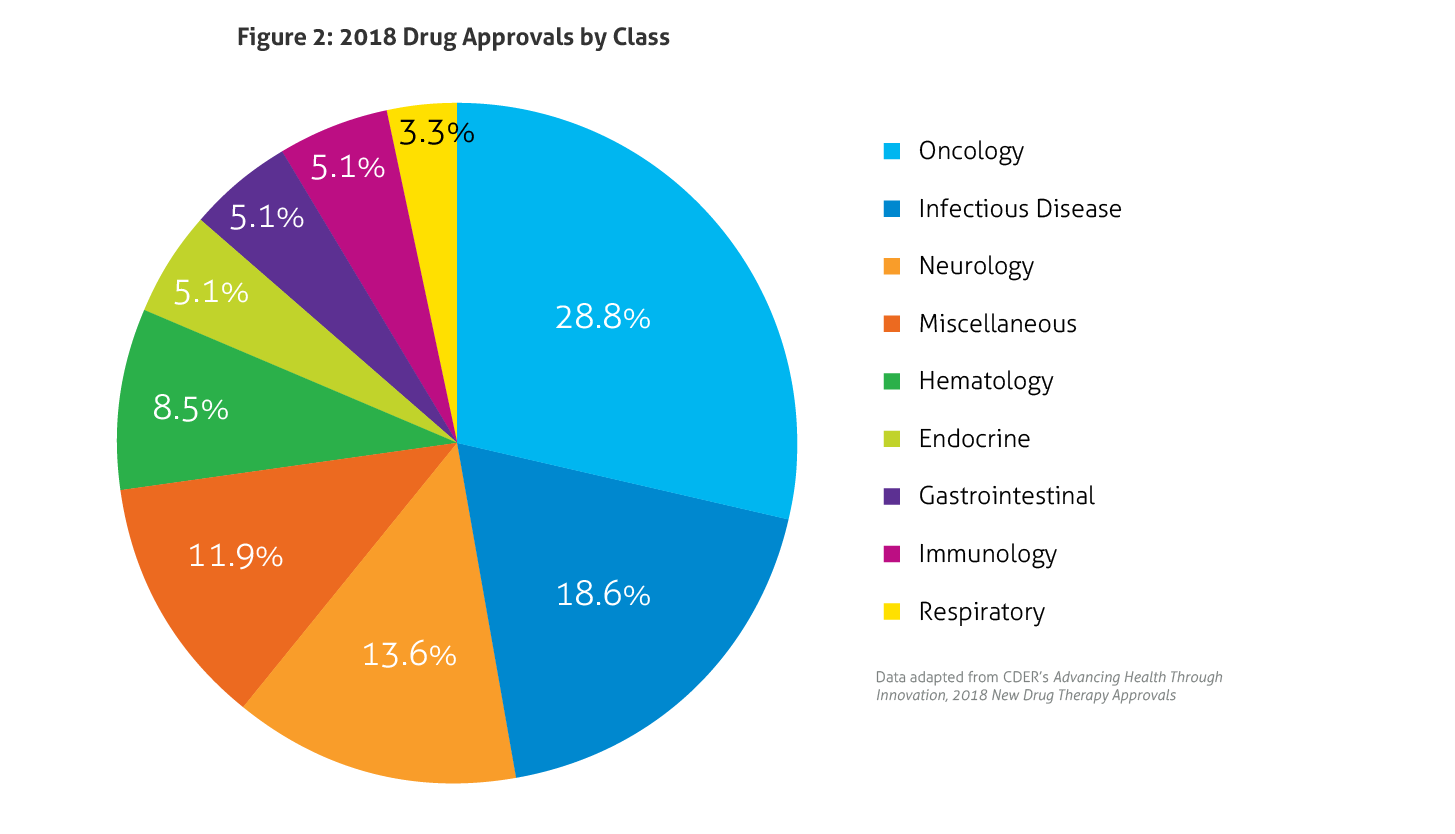 Some of the notable 2018 approvals included the first non-opioid drug approved to reduce opioid withdrawal symptoms, a new antiretroviral for multidrug resistant human immunodeficiency virus-1, a new class of drugs for migraine (calcitonin gene-related peptide receptor antagonists), the first FDA-approved drug derived from marijuana, the first treatment approved for multiple sclerosis in children, expanded options for cystic fibrosis, and the first antibiotic approved under the Limited Population Pathway for Antibacterial and Antifungal Drugs.
Some of the notable 2018 approvals included the first non-opioid drug approved to reduce opioid withdrawal symptoms, a new antiretroviral for multidrug resistant human immunodeficiency virus-1, a new class of drugs for migraine (calcitonin gene-related peptide receptor antagonists), the first FDA-approved drug derived from marijuana, the first treatment approved for multiple sclerosis in children, expanded options for cystic fibrosis, and the first antibiotic approved under the Limited Population Pathway for Antibacterial and Antifungal Drugs.