As a market leader and disruptor in specialty drug management, Magellan Rx Management has been delivering targeted and innovative solutions for over 16 years to help health plans reduce specialty drug costs on the medical benefit while maintaining a high quality of care for their members. Our suite of solutions can help plans develop customizable, flexible programs to meet some of their toughest challenges.
- Prior authorization: Ensures complex and high-cost drugs are prescribed according to evidence-based policies.
- Post-service pre-payment claims edits: Assures medical benefit drugs are paid correctly.
- Provider network strategy: Encourages lower-cost but equally effective agents through a variable fee schedule.
- Site of service management: Guides medical injectable drug administration to lower-cost and clinically appropriate site of care.
- Medical formulary management: Enhances management of medical drug classes to promote the most cost-effective therapies
Why medical pharmacy management matters
With specialty drug costs accounting for nearly half of total drug spend, health plans continue to look for better ways to manage those rising costs while staying ahead of ever-changing market dynamics (like emerging therapies for rare and orphan diseases and new-to-market biosimilars). Specialty drugs administered by healthcare professionals (typically in a provider’s office, hospital outpatient facility, or through home infusion) are paid under the medical benefit—or what we like to call “medical pharmacy”—and remain a leading driver of rising costs. In fact, according to our research, the latest five-year per-member-per-month (PMPM) trend for medical pharmacy spend was 65% in Commercial, 40% in Medicare, and 78% in Medicaid.
A real-life customized solution
One of our health plan customers with a mix of Commercial, Medicare & Medicaid lives was beginning to see significant utilization in specialty medications. They turned to Magellan Rx’s clinical and pharmacy trend experts, who analyzed trend drivers, recommended a multi-pronged approach to management based on their unique data, and collaborated with the plan to implement several programs to maximize effectiveness and meet plan goals including innovative strategies such as a drug wastage solution.
So, what are the results?
Our health plan partner realized a cost reduction in just one year by implementing a suite of solutions alongside our team of medical pharmacy experts—resulting in a nine percent decrease in medical drug spend! Based on this particular’s plan size and benefit design, each solution contributed demonstrably to overall savings.
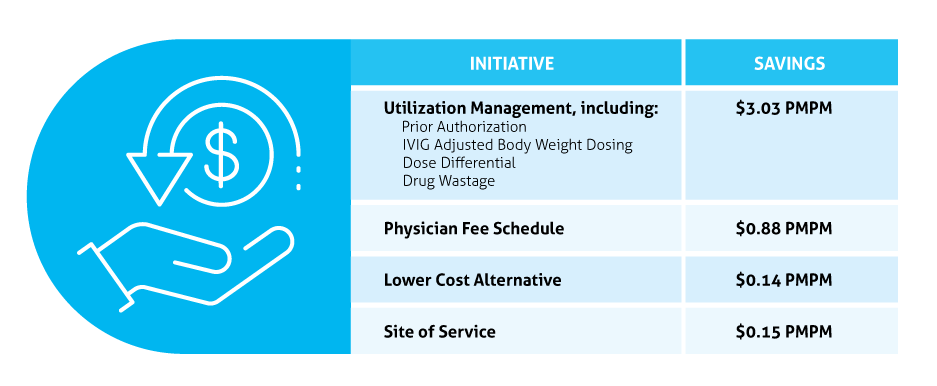
Individual program implementation is dependent on plan size and other factors. These flexible solutions can also operate outside of the traditional payer-PBM relationship. Now, you can plug in to the extensive clinical expertise and experience at Magellan Rx by delegating specialty and medical drug management services while retaining a separate pharmacy benefit manager.
Are you looking for a customizable, flexible solution to combat rising specialty spend? Connect with us today!





